Motiva
JW BREAST SURGERY
01 Motiva is a Natural Shape
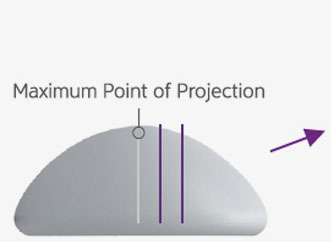
Thanks to the fluidity of Progressive Gel Ultima™, the implant changes shape naturally with the movement of the body taking on a teardrop shape when standing and a soft, rounded shape when lying down.
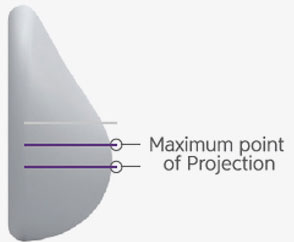
When Lying Down
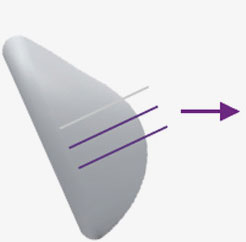
When Sitting
When Standing
Natural changes in breast shape that move together with the body just like real breasts.
02
Motiva: Soft to the Touch
Cell-Friendly Surface
The uniform outer shell made with 3D imprinting technology features a smooth silk surface that helps reduce inflammation during capsule formation after surgery. Through a carefully controlled manufacturing process, the implant surface is made cell-friendly, lowering the risk of capsular contracture and providing an exceptionally soft texture. It also promotes natural interaction between the implant and body tissue, resulting in minimal foreign body reaction.
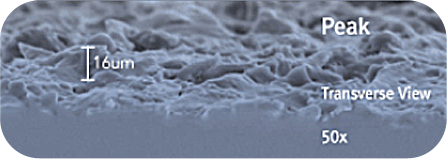
Surface
360°
Surface Consistency
50x
3
03 Motiva is Safe
Bluseal (Bluseal Barrier – Layer)
The Bluseal technology prevents the gel from leaking or spreading to other parts of the body.
Reduced risk of gel diffusion
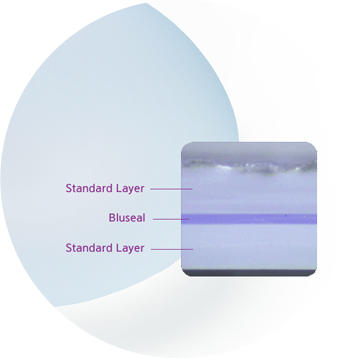
Reduced risk of capsular contracture
4
04 Motiva is Durable
As it is manufactured with uniform thickness and viscoelasticity across the entire 360° surface, it offers excellent elasticity and durability under equal tensile strength. In addition, the implant has a low risk of damage during insertion and can be placed through a smaller incision.

JW BREAST SURGERY
JW Plastic Surgery’s Breast Augmentation Story
01
We are a Plastic Surgery Clinic Recommended by Other Medical Professionals
- Over 21 years of extensive experience and expertise
- A trusted breast revision surgery center recommended by other hospital doctors
- Ongoing breast surgery research through academic conferences and presentations
- 1:1 dedicated care system designed to prevent risk of secondary revision surgeries
- A renowned specialist in 4K UHD endoscopic breast augmentation

02
Pre-Surgery ONE-STOP Comprehensive Examination
Before breast surgery, all necessary health assessments, including blood tests, EKG, and chest X-ray can be performed conveniently in-house at JW clinic without needing to visit other hospitals such as an internal medicine clinic.
Blood test

Electrocardiogram (ECG)
Chest X-ray
Motiva divina™ Virtual Simulation

At JW Plastic Surgery, we use a 3D body scanner to provide accurate diagnosis and predict precise surgical outcomes.
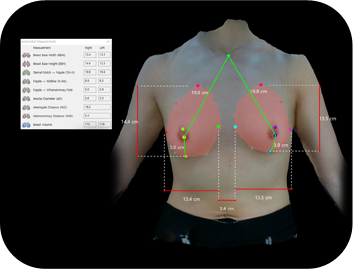
Accurate measurement of body dimensions
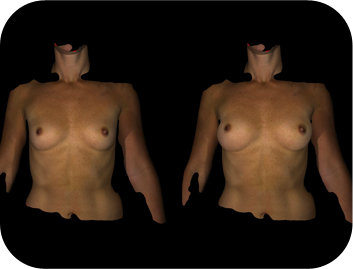
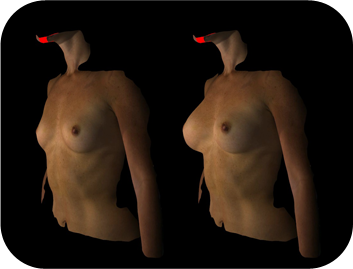
Detailed 3D image analysis for precise surgical planning
03
Implant Fitting Simulation
This program allows patients to try on implants that suit their body type using a special fitting bra, so they can have an idea of the size and shape of their breasts after surgery.

STEP 01
Accurate breast size measurement

STEP 02
Implant fitting

STEP 03
Check breast fit and appearance
04
Postoperative Breast Surgery Care System
All treatments and follow-ups are personally performed by the operating surgeon.
Day 1 post-surgery
Check for any bleeding and perform the first treatment.
Day 2~3 post-surgery
We apply waterproof tape to the incision site. (Full-body showers are allowed from this day.)
7 Days After Surgery
All tapes are removed. Since no skin sutures are used, stitch removal is unnecessary, and there are no suture-related scars.
1 Month Post-Surgery
Prescription of scar cream and whitening cream.
Patients can switch from a surgical bra to a regular bra.
(It is recommended to choose a bra that does not affect breast shape.)
Every 3 Months
Continuous follow-ups, up to 1 year
After 1 Year
Regular check-ups are no longer needed, but patients can continue to receive follow-up evaluations from their surgeon at any time after.

LED Light Therapy
Promotes blood circulation and romotes deswelling

High-Frequency Thermal Therapy
Promotes blood circulation and reduces swelling

Capsulitis Treatment
Prevents capsular contracture, relieves swelling and pain
Breast Ultrasound
Implant check

Hematoma Laser & Injection
Hematoma treatment

Scar Whitening Laser
Treats pigmentation caused by hematoma
Prescription of Special Medication
After surgery, if necessary, special medications may be prescribed to achieve a natural breast appearance. These medications are carefully selected based on clinical research and help minimize capsular contracture, even in patients who are prone to developing it due to their body type.
Wearing a Special Surgical Bra
Even if both breasts are made as symmetrical as possible during breast augmentation surgery, the position of the implants may shift over time depending on lifestyle habits or the natural characteristics of the breast tissue.
For example, right-handed people tend to use their right arm and pectoral muscles more frequently, and since the heart is located on the left side, the height and angle of the rib cage differ slightly between sides.
The surgical bra helps maintain proper implant positioning, correcting any imbalance and providing consistent support to prevent displacement.
In addition, after augmentation surgery, the inframammary fold can sometimes appear less defined, creating an unnatural look. The surgical bra helps redefine the fold and expand the lower breast area, enhancing the overall natural appearance of the breasts.
JW Plastic Surgery provides this special surgical bra free of charge,
and during each follow-up visit, the bra is adjusted and customized to fit the patient’s breast shape perfectly.
Surgical Safety Management System
01
Infection prevention through a thorough sterilization protocol
Equipped with an air shower cubicle, sterilization and disinfection equipment, HEPA filters, and a laminar flow air purification system meeting high-risk surgery standards to prevent infection.
02
Minimizing capsular contracture through aseptic clean surgery
Continuous monitoring of the patient’s ECG, blood pressure, pulse, oxygen saturation, carbon dioxide levels, and body temperature throughout the procedure.
03
Real-time patient monitoring system during surgery
Equipped with an uninterrupted power supply and fire-resistant structure throughout the entire hospital building.
04
Prepared for any emergency situation
Emergency treatment system equipped with a defibrillator and emergency rescue equipment.
05
Emergency Response System
Various implants available, including Motiva, Mentor, and Sebbin are selected according to each individual’s breast characteristics and personal preferences.
06
Wide range of clinically proven implants
Our in-house anesthesiologist provides care from the beginning of surgery through recovery, with safety equipment in place to respond immediately to emergencies and ensure effective postoperative pain management.
05
Best Q&A About Breast Augmentation Surgery
Breast implants are not inserted within the mammary gland tissue itself, but rather under the mammary glands or under the pectoral muscle.
Therefore, they do not affect the mammary glands or milk ducts, which are responsible for milk production and secretion.
As a result, breastfeeding is possible even after surgery.
For the same reason, breast implants do not interfere with breast cancer screening or tumor detection within the mammary tissue.
When an implant is placed in the body, a thin layer of scar tissue naturally forms around it, it is called a capsule. All patients who receive implants develop this capsule. Capsular contracture refers to a condition where this capsule becomes abnormally thick and tightens around the implant.
A severe form, known as spherical (grade IV) capsular contracture, occurs when the breast becomes hard and round in shape, making it look unnatural.
It can develop if excess bleeding or infection occurs at the surgical site, or if the patient’s body reacts strongly to the implant due to individual sensitivity.
To prevent this, thorough hemostasis and sterilization must be performed during surgery, and the pocket for the implant must be dissected accurately. Postoperative anti-contracture medication may also be prescribed.
If a classic smooth implant is used, post-surgery massage may be required; however, implants with a textured or treated surface have built-in resistance to capsular contracture, massage is not necessary.
There is no fixed lifespan for implants, so regular replacement is not necessary. Unless a rupture or other major issue occurs, the implants can last a lifetime. In the past, older implants often ruptured after around 10 years, but modern implants have a far longer lifespan, and the rupture rate is very low.
To determine the right implant, the patient first tries on external sizers inside a bra to estimate the preferred size. Then, the width of the patient’s chest is measured to determine the appropriate implant diameter.
Among implants with that diameter, several size options close to the patient’s preference are selected.
During surgery, a temporary implant (sizer) is placed first, and the patient’s body is positioned upright on the operating table to simulate the result.
Based on appearance and balance, the final implant size that best fits the patient’s body and preference is chosen and inserted.
There are various implant brands such as Motiva, Sebbin, and Mentor.
Each has its own advantages and characteristics,so the most suitable one is selected after an in-depth consultation with the patient.
There are several incision types for breast augmentation:
axillary (armpit), areolar (around the nipple), inframammary (under the breast fold), and trans umbilical (through the navel).
Areolar and navel incisions are less commonly used today due to certain drawbacks, while axillary and inframammary incisions are the most widely performed methods.
The axillary incision is mainly used for younger or unmarried women with small breasts and shallow folds.
The scar can be hidden in the armpit crease, leaving it barely visible.
The inframammary incision allows faster recovery and is advantageous for correcting sagging or constricted breasts.
When performed on patients with a deep breast fold or post-pregnancy changes, scarring is minimal.
In the inframammary incision method, since the incision is close to the breast, the internal area can be seen directly with lighting alone, so surgery can be performed accurately without an endoscope.
However, in the traditional axillary incision method, the incision is farther from the breast, making it difficult to see inside. Surgeons must use a long metal dissector to create the implant pocket, which can lead to less precise dissection, more bleeding, and greater pain.
As opposed to the 4K UHD endoscopic axillary method, a high-resolution endoscope provides a clear internal view of the breast.
Dissection is performed precisely using radiofrequency equipment, resulting in minimal bleeding, reduced pain, and faster recovery.

